What is a Biologic?
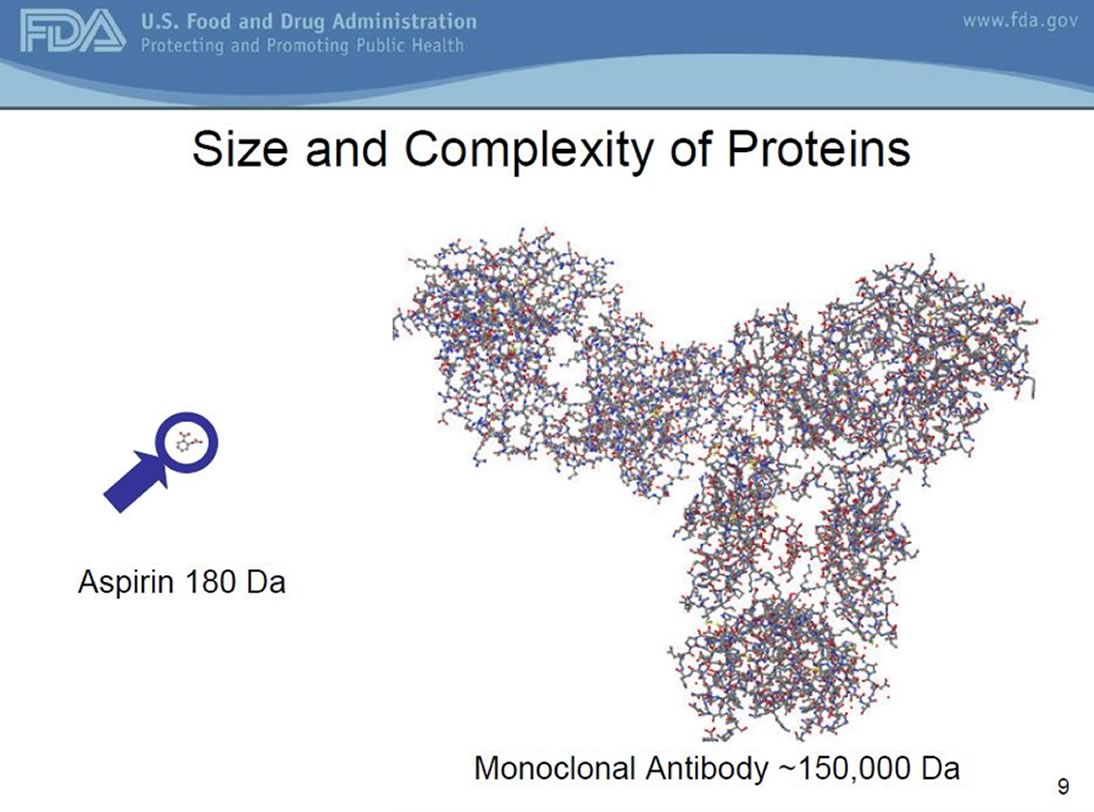
Biologics, also known as the ‘reference drugs’, are biochemically engineered large proteins with a very complex structure. Given their structural requirements, they must be produced inside living cells such as bacteria or yeast. This is in contrast to small molecule drugs (i.e. Aspirin), which can be made using highly reproducible techniques outside of living cells, in a laboratory setting.
FDA – Overview of Biological Products
What Is a Biosimilar? What makes it “Similar” to a Biologic?
A biosimilar is a drug that is determined to be highly similar to the reference drug. It is important to keep in mind that a biosimilar can never be identical to the reference drug, given the mechanism by which they are produced. Furthermore, it is not even possible for each manufactured lot of the same reference drug to be identical to each other. Proteins are very large, complex structures that cannot be identically reproduced, even within the same cell line.
What Conditions Do Biologics and Biosimilars Treat?
Biologics and biosimilars are used to treat a multitude of conditions. Some examples include: anemia, diabetes, inflammatory bowel disease, psoriasis, rheumatoid arthritis and some forms of cancer. Often times, biologics can be used to treat more than one condition (also known as an indication). Any given biosimilar may be used to treat all or some of the reference drug’s indications. The indications authorized for a biosimilar is dependent on a multitude of factors. For example, Health Canada may choose not to authorize the use of the biosimilar for a shared indication with the reference drug, due to lack of scientific evidence or risk/benefit analysis.
What are Risks and Benefits of Using Biologics and Biosimilars?
The emergence of biologics and biosimilars has dramatically changed the landscape that clinicians use to treat their patients. These drugs are much more targeted to specific pathways in the body, thereby allowing targeted treatment with improved outcomes. As with any therapy, biologics and biosimilars also carry risks such as a compromised immune system. It is always important to speak to your health care provider about the steps you need to take before and during your treatment with biologic and biosimilar therapy.
It is also worth discussing immunogenicity at this time. By nature, our immune system has evolved to recognize and attack foreign (i.e. ‘not-self’) proteins. Therefore, when biologics or biosimilars are introduced into our body, the natural response is for our body to react to them. This is referred to as the immunogenicity of the product. Given what has previously been mentioned about the inability to identically reproduce biologics, a patient can react to any administration of a reference biologic, a switch from a reference biologic to a biosimilar, or any administration of a biosimilar.
How are Biosimilars Regulated by Health Canada?
Biosimilars are regulated under the Food and Drugs Act and the Food and Drugs Regulations. They are approved based on a comparison to the reference drug. They must be shown to have no clinically significant or meaningful differences to the reference drug in terms of safety (i.e. adverse event profile) and efficacy (i.e. how well they work when used for treatment). Health Canada has developed a very comprehensive and rigorous scientific framework that reflects that of other regulatory bodies around the world. Given this, the goal is to have patients and clinicians feel confident in the use of biosimilars, just as they would in the use of their reference biologic.
How Do Clinicians and Patients Access Biologics and Biosimilars?
When Health Canada approves the sale of a biologic or biosimilar, this does not necessarily translate to drug funding through federal, provincial, territorial or private drug plans. Each party is responsible for reviewing the entry of the new drug and will make a decision as to whether or not patient funding will be provided. Generally, the cost associated with research, development and production of a biosimilar is less than the cost associated with the reference drug. Therefore, biosimilars are made available to consumers at a much lower cost. This makes their use and uptake enticing, given the need for efficient health care dollar allocation.
What Are the Sales Associated with Biologic drugs?
The sales market for biologics has dramatically grown from $0.8 billion in 2006 to $3.6 billion by 2016. The sales account for 15.9% of Canada’s pharmaceutical sales. The Canadian market is also highly concentrated, with the top 5 biologic drugs (infliximab, adalimumab, ranibizumab, etanercept and insulin glargine) accounting for 11.4% of the total pharmaceutical sales in Canada in 2016.
What is the role of the Pharmacist?
At this time, Health Canada’s approval of a biosimilar is not an announcement of equivalency. That is to say, if a patient is given a prescription for a reference biologic, the pharmacist cannot dispense the lower cost biosimilar. The patient would have to be issued a new prescription from the physician for the biosimilar. This is in contrast to the pharmacists’ practice guidelines for generic drugs. For example, if a physician prescribes Pantoloc for acid reflux, the pharmacist is required to dispense the lowest cost equivalent, pantoprazole sodium. This mandatory substitution is explained in the Drug Interchangeability and Dispensing Fee Act (DIDFA). The difference in practice guidelines goes back to the biologic and biosimilar manufacturing process. A biosimilar is not a generic equivalent of the reference biologic, and therefore cannot be automatically substituted.
References
- Ensuring Better Value for Money: Expanding Interchangeability and Off-Formulary Interchangeability Progress. (2013 January). Ministry of Health and Long-Term Care Ontario. Retrieved from: http://www.health.gov.on.ca/en/pro/programs/drugs/plan_reform_ods/ensuring_expand_interchangeability.aspx
- Fact Sheet: Biosimilars. (2017 August). Government of Canada. Retrieved from: https://www.canada.ca/en/health-canada/services/drugs-health-products/biologics-radiopharmaceuticals-genetic-therapies/applications-submissions/guidance-documents/fact-sheet-biosimilars.html
- Potential Savings from Biosimilars in Canada. (2016). Patented Medicine Prices Review Board. Retrieved from: http://www.pmprb-cepmb.gc.ca/CMFiles/NPDUIS/2017_Conference_Posters/post_6_biosim.pdf
Suggest a topic
Do you have a question for the pharmacist or a topic suggestion?
Send us an email and suggest a topic.
This article was provided by Daniella Santaera, Clinical Pharmacist for RXI Specialty Pharmacy in association with Rx Infinity. Rx Infinity provides optimal and sustainable patient management solutions through customized programs, innovative technology and added value services that improve the overall patient experience; while helping payers and plan sponsors achieve sustainability in the management of drug plans expenditures.
This information is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified health provider with any questions about your medical condition. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.