About Opioids
Opioids are drugs that are traditionally prescribed by physicians to patients for the treatment of pain. It is important to note that when opioids are used as prescribed, their potential for abuse is quite low. However, if taken at higher than prescribed doses and at inappropriate dosing intervals, the risk of abuse increases. This is due to their potential to cause euphoria (“high”) in the patient. Anyone who is using opioids can experience an overdose. However, there are other factors other than opioid misuse that can increase the risk of experiencing an overdose. These include:
- Taking opioids with alcohol or other sedatives
- Injecting drugs
- Using drugs of unknown purity or strength
- Other health conditions such as liver or kidney disease, or breathing issues
The Opioid Crisis
Unfortunately, over the recent years, there has a been a dramatic increase in number of cases of opioid-related illness and death. Public Health Ontario has gathered data over many years depicting this rise. Notably, the greatest rise has been over the last 2 years.
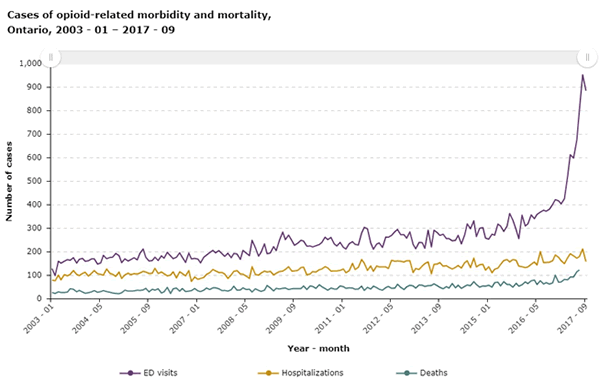
The Government of Canada released a report highlighting approximately 2,816 opioid related deaths in Canada in 2016. The majority of these deaths involved one or more non-opioid substances (i.e. alcohol, benzodiazepines)1.
Signs and Symptoms of an Opioid Overdose
It is extremely important to recognize the signs and symptoms of an opioid overdose, as an overdose is potentially fatal medical emergency. Signs of symptoms may include:
- Extreme drowsiness or difficulty talking
- Blue lips or nails
- Very small pupils
- Cold and sweaty skin
- Dizziness and confusion
- Choking or gurgling sounds
- Vomiting
- Slow, weak or no breathing
- Inability to wake up, even when shaken or shouted at
The Solution – Naloxone
Naloxone is a lifesaving medication. Its mechanism of action involves displacement and prevention of the binding of opioids to receptors in the body, thereby reversing their effects. Given this mechanism of action, administering naloxone can precipitate symptoms of acute opioid withdrawal. Symptoms may include (pain, increased blood pressure, sweating, agitation, vomiting, seizures, respiratory distress syndrome). Conversely, naloxone will not reverse respiratory depression caused by non-opioid drugs. It also does not have any abuse potential.
The onset of action depends on the route of administration. For the intramuscular injection, the onset of action is 6 minutes. For the intranasal administration, the onset of action is 4 minutes. The duration of action can range from 20-90 minutes and depends on the route of administration as well as the type and dose of the opioid the person has taken. As a result, naloxone provides temporary but safe and effective relief of an overdose
What is Included in the Naloxone Kit and What are the Administration Steps?
There are two publicly funded Naloxone Kits available.
| Kit Type | ||
| Components | Nasal Spray | Intramuscular Injection |
| One hard carrying case | ✓ | ✓ |
| Two doses of Narcan spray (4 mg/0.1 mL) | ✓ | |
| Two 1 mL ampoules or vials of naloxone hydrochloride 0.4 mg/mL injection | ✓ | |
| Two safety engineered syringes with 25 gauge 1 inch needles attached | ✓ | |
| Two safe ampoule opening devices (snappers or openers) as applicable | ✓ | |
| One pair of non-latex gloves | ✓ | ✓ |
| One card that identifies: • person trained to give naloxone • date that the kit was supplied • expiry date of the naloxone | ✓ | ✓ |
| One instructional insert | ✓ | ✓ |
5 Steps to Save a Life
Toronto Public Health’s “5 Steps to Save a Life”, is a great tool to aid in attending to an opioid overdose emergency. This was created through their POINT (Prevent Overdose in Toronto) program. It is very important to stay with the person throughout these 5 steps:
- STEP 1 – Shout the person’s name and shake their shoulders
- STEP 2 – Call 9-1-1 if unresponsive
- STEP 3 – Administer Naloxone (1 spray into the nostril or 1 ampoule into the arms or legs)
- STEP 4 – Start CPR (chest compressions and/or rescue breathing if trained)
- STEP 5 – Is it working? If no response in 2-3 minutes, repeat steps 3 and 4
Who Is Eligible to Receive a Publicly Funded Naloxone Kit and Where Can The Public Get One?
The Ministry of Health and Long-Term Care released a statement in June 2016, that Ontario is allowing the availability of Naloxone in pharmacies at no cost and without a prescription. This resulted from NAPRAs (National Association of Pharmacy Regulatory Authorities) reclassification of Naloxone from a Schedule I to Schedule II drug only “when indicated for emergency use for opioid overdose outside hospital settings”2. This was officially implement in February 2017.
The following is a list of people who are eligible to receive a Naloxone Kit
- Current opioid user at any dose
- Past opioid user who is at high risk of returning to opioid use
- A family member or friend who is at risk of an opioid overdose
There must also be an understanding that the person who may require the use of naloxone have no contraindications to naloxone such as a known hypersensitivity.
It is the responsibility of the pharmacist to provide the appropriate training to the eligible persons. The Ontario government compiles and maintains and list of community pharmacies, community programs and provincial correctional facilities that are able to supply the public with naloxone kits. If a pharmacy is not on the list, they are able to email their request to Public Drug Programs.
Additional Resources
For more information on POINT training, please visit https://www.toronto.ca/community-people/health-wellness-care/health-programs-advice/overdose-resources-become-a-partner-agency/take-home-naloxone-program/
References
- Canadian Centre on Substance Use and Addiction. (2017 September). Canadian Drug Summary: Prescription Opioids. Retrieved from: http://www.ccdus.ca/Resource%20Library/CCSA-Canadian-Drug-Summary-Prescription-Opioids-2017-en.pdf#search=%22prescription%20opioids%22
- Government of Canada. (2016 March 22). Notice: Prescription Drug List (PDL): Naloxone. Retrieved from: https://www.canada.ca/en/health-canada/services/drugs-health-products/drug-products/prescription-drug-list/notice-naloxone.html
- Ministry of Health and Long-Term Care. (Accessed 2018, May 1). Naloxone Frequently Asked Questions. Retrieved from http://www.health.gov.on.ca/en/pro/programs/drugs/naloxone/naloxone_faq.aspx
- Government of Canada. (2017, August 3). Opioid Overdose. Retrieved from https://www.canada.ca/en/health-canada/services/substance-abuse/prescription-drug-abuse/opioids/overdose.html
- Government of Canada (2018, April 9). About Opioids. Retrieved from https://www.canada.ca/en/health-canada/services/substance-abuse/prescription-drug-abuse/opioids/about.html
This article was provided by Daniella Santaera, Clinical Pharmacist for RXI Specialty Pharmacy in association with Rx Infinity. Rx Infinity provides optimal and sustainable patient management solutions through customized programs, innovative technology and added value services that improve the overall patient experience; while helping payers and plan sponsors achieve sustainability in the management of drug plans expenditures.
This information is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified health provider with any questions about your medical condition. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.